Canada, like many countries worldwide, has seen rapid growth over the past decade in patient[1] engagement efforts at all levels of the health system. This has reached beyond the direct patient-provider interface to expectations of involvement for organisational and system-level change, as well as in domains of policy-making, research, and education. At its core, engaging with patients recognizes their untapped potential, acknowledging their lived experience of illness and of care as legitimate forms of knowledge where they have gained ‘expertise by experience’. The potential of harnessing this knowledge through engagement efforts is seen to be one of the key levers for transforming the health system for high quality, patient-centred care (Reinertsen et al., 2008).
The role of a pan-Canadian health organisation to support patient engagement
As a newly amalgamated organization with a relentless focus on improving healthcare, with – and for – everyone in Canada, Healthcare Excellence Canada (HEC) has a role in building, supporting, and sustaining patient engagement for health system improvement. Healthcare Excellence Canada has made concerted efforts to raise the voices of patients to improve the safety and quality of care. The concept of ‘engagement-capable environments’ emerged through work supported by CFHI in specific learning collaboratives (Patient, Family and Caregiver Engagement (cfhi-fcass.ca), working with healthcare organisations across Canada to embed meaningful and authentic patient engagement in quality improvement initiatives (Fancott et al,, 2018). Patient engagement has now become an expectation across HEC activities and programs to support meaningful change in the healthcare system and the growth of engagement capable environments for quality and safety. We support capacity development of patient partners, healthcare teams and leaders and have co-developed numerous resources to share lessons learned from varying perspectives. Open access, freely available resources and practical tools from Canada and worldwide are housed on our Patient Engagement Resource Hub to support meaningful engagement practices across the health system (Patient Engagement Resource Hub (cfhi-fcass.ca).
What are ‘engagement-capable environments’?
An understanding of meaningful and authentic engagement began to emerge in evaluation work that examined early patient engagement learning collaboratives, and deepened through exploration of additional case studies of healthcare organizations and networks in Canada, the United States and United Kingdom (Baker et al, 2016a). Engagement capable environments are those that have embedded the values of patient-centred and patient-partnered care as the philosophy of care that underlies the priorities of the organization. These organizations have created the necessary infrastructures to support ongoing and active engagement of patients, together with staff, healthcare teams and leaders at all levels of care, and built on principles of relationships, respect and reciprocity to create a culture of engagement. In the words of a wise patient partner: “To my mind, engagement capable environments are those that have a heart.” (Anya Humphrey, in Fancott et al., 2018).
Three key pillars form the foundation of engagement capable environments and are interrelated, interdependent, and mutually reinforcing (Baker et al., 2016b). First, engagement capable environments create the space for and build capacity of patient partners. Recruitment and orientation efforts support the ability of patient partners to work with teams, where there is clarity in shared purpose, roles, and expectations of all involved. Patient partners are prepared and feel supported in their roles, and barriers to participate are removed.
Second, while there was emphasis on recruitment and preparation of patient partners for engagement, equally so, there is need to prepare and support staff and healthcare teams to engage with patients. Staff and teams need to learn to work with patients in new and different ways, with an openness to listen and to learn together, thereby reshaping relationships and decision-making processes. Recognizing and valuing the lived experience and unique insights that patients offer is key to rethinking what shared solutions may be possible. Safety must be created so that everyone can ‘speak their truth.’
Third, leaders walk the talk of engagement and role model behaviours that indicate how patient experience is not only valued but sought out. They set expectations and accountabilities for patient engagement and how patients are welcomed at all levels of the organization, at the direct care level through to governance tables. Patient engagement is a priority that is aligned with strategy, and patient-centred care is an embedded philosophy of care. Leaders understand that purposeful and authentic engagement does not happen by itself but rather requires the appropriate resources and the development of infrastructures to support consistent engagement efforts across the organization.
Figure 1: Engagement-capable environments
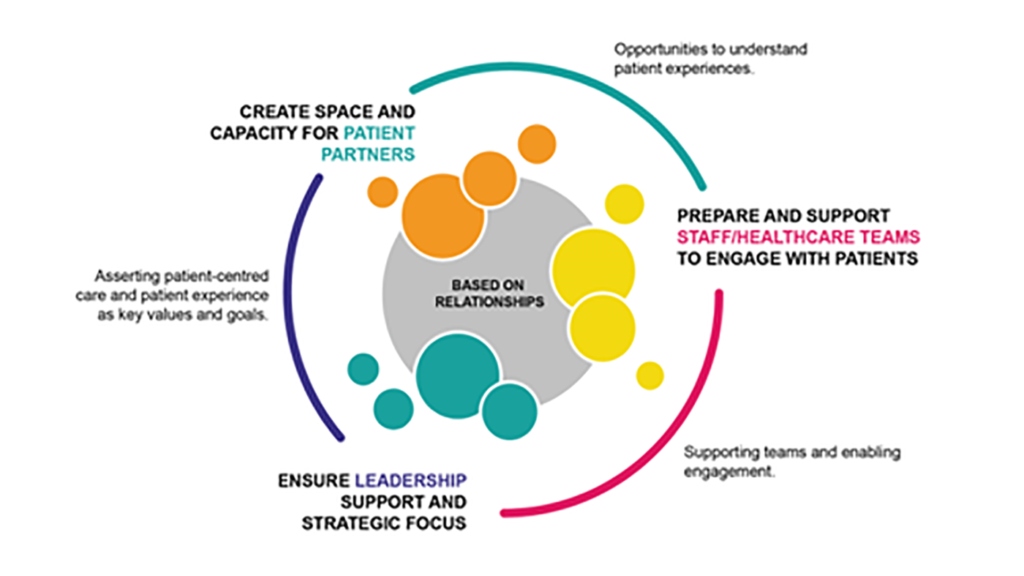
(Adapted from Baker and Denis, 2011; Baker et al., 2016b)
The evolution of engagement-capable environments
Through this current pandemic, there is need to strengthen and evolve engagement-capable environments to ensure patient-centred and partnered principles remain at the core of the health system. In particular, the devastating effects of Covid-19 has shone a light on issues of existing social and health inequities, further exacerbated by the pandemic. It draws attention to the need to widen our circles of engagement, to become more diverse and inclusive of populations that are more representative of those requiring services, and to consider more equitable forms of engagement. The distribution of power is central to collaborative/partnership models of engagement with shared leadership. Engagement-capable environments support this shift from ‘old power’ to ‘new power’ (Heimans and Timms, 2014) as engagement efforts become a social movement (Bibby et al., 2009), creating a ‘push-pull’ where patients and families see the power of their knowledge gained through lived experience, have expectations to be involved and to partner in decision-making processes that support improvement in their care and across the health system. Engagement capable environments need to further demonstrate their impacts, making links to positive patient, family and provider experience, better use of resources, and improved outcomes that come through engagement approaches.
Purposeful and authentic engagement is just that: it has intention, it has meaning, and it feels real to those involved. It takes work to support engagement in this way, not as a series of checkboxes. Becoming an engagement capable environment is a journey that transforms the culture of healthcare organizations and health systems that will truly focus on the needs and priorities of those it serves.
[1] While the term ‘patient’ is used throughout this article, it refers to those with lived experience of the health system including patients, residents, clients, consumers, as well as family members and caregivers.
About the author
 Carol Fancott is the Director of Patient Partnership and Engagement at Healthcare Excellence Canada. She leads the development, delivery, and evaluation of patient engagement programs, designed to improve the patient experience and quality of care. Carol is a physiotherapist by clinical training and has held many roles as a clinician, educator, researcher, and health leader. She obtained a PhD at the Institute of Health Policy, Management, and Evaluation at the University of Toronto. Her doctorate explored how healthcare organizations gather and utilise the experiences of patients and families through storytelling methods for organisational learning and improvement to change processes and systems of care.
Carol Fancott is the Director of Patient Partnership and Engagement at Healthcare Excellence Canada. She leads the development, delivery, and evaluation of patient engagement programs, designed to improve the patient experience and quality of care. Carol is a physiotherapist by clinical training and has held many roles as a clinician, educator, researcher, and health leader. She obtained a PhD at the Institute of Health Policy, Management, and Evaluation at the University of Toronto. Her doctorate explored how healthcare organizations gather and utilise the experiences of patients and families through storytelling methods for organisational learning and improvement to change processes and systems of care.
References:
Baker, G.R. and Denis, J-L. (2011). Patient engagement and system transformation. Presentation to Patient Engagement Workshop, Edmonton, AB, November 2011.
Baker, G.R., Judd, M., and Maika, C. (2016a). Patient Engagement: Catalyzing improvement and innovation in healthcare, Toronto, On: Longwoods Publishing Corporation.
Baker, G.R., Judd, M., Fancott, C. and Maika, C. (2016b). Creating engagement capable environments in healthcare. In G.R. Baker, M. Judd and C. Maika, eds. Patient Engagement: Catalyzing improvement and innovation in healthcare, Toronto, On: Longwoods Publishing Corporation, 11-34).
Bibby, J., Bevan, H., Carter, E., Bate, P., and Robert, G. (2009). The power of one, the power of many: Bringing social movement thinking to health and healthcare improvement. Coventry, UK: NS Institute for Innovation and Improvement.
Fancott, C., Baker, G.R., Judd, M., Humphrey, A., and Morin, A. (2018). Supporting patient and family engagement for healthcare improvement: Reflections on ‘engagement capable environments’ in pan-Canadian learning collaboratives. Healthcare Quarterly, Vol 21 (special issue), 12-20.
Heimans, J. and Timms, H. (2014) Understanding ‘new power’. (2014). Harvard Business Review (Dec), 49-56.
Reinertsen, J.R., Bisognano, M., and Pugh, M.D. (2008). Seven leadership leverage points for organization-level improvement of healthcare (2nd edition). Cambridge, MA: Institute for Healthcare Improvement.
