The health of Australia’s young people is crucial to the ongoing prosperity and connectedness of our society. What steps we take now have long-term impacts not only on health outcomes for the parents of tomorrow, but also on the future social and economic wellbeing of Australia.
The period from adolescence to young adulthood forms a critical life stage. Young people acquire necessary emotional skills and cognitive abilities for independence, form intimate relationships, complete education, transition to employment and discover their true identity. This period may be fraught with a number of different health challenges, which, if not supported by a contemporary and responsive healthcare system, can lead to catastrophe.
Even before COVID-19 reared its ugly head, young Australians were battling in more ways than one. They are in danger of being the first generation to have lower living standards than their parents’ generation. No, it’s not smashed avos and oat milk lattes causing their stagnating wealth. Economic pressures on young adults have been amplified by wage stagnation and rising under-employment, deepening intergenerational inequalities. This leads to unprecedentedly high levels of financial stress and potentially even social exclusion.
What’s more, a socioeconomic disadvantage in making the transition from school to further education or work is becoming entrenched. One in five young Australians are not fully engaged in education or employment, but that figure is much higher in those from poorer neighbourhoods and regional Australia. Factors including insufficient secure housing, lack of understanding of career pathways, the use of drugs and alcohol and a dysfunctional family life can hinder this transition greatly.
Mental health inquiries are more frequent than iPhone updates, yet … we seem to be going backwards.
Needless to say, the overall mental health profiles of our young people remain poor, with almost a quarter (23%) of those aged 18-24 reporting high levels of mental distress. A study by the Australian Bureau of Statistics reported that of the 20% who admitted having these feelings in June of 2021, only 15% had discussed those feelings with a doctor or health professional. Statistically, this suggests 25% of people are not willing to reach out for professional help.
In the area of youth mental health, 15 years of investment appears to have done little. Mental health inquiries are more frequent than iPhone updates, yet on many indicators, we seem to be going backwards. Blaming governments is a natural response for this decline. However, it’s hard to fault Australian governments when they’ve made radical changes to major health programs like Medicare to increase access to services as well as establish bodies to oversee various policies and programs.
Given Australia’s short political cycle, ministers responsible for launching inquiries are often not around to receive the report and implement the proposed recommendations. It’s also true that the adoption of these recommendations has been patchy; instead of acknowledging the need for a comprehensive, community-driven approach to mental health, governments have predominantly focused on the easier-to-implement options and shied away from the more challenging.
Ian Hickie, former national mental health commissioner, suggests that the first task for any new inquiry should be to identify “high value targets” like early intervention, increased support in regional areas and the use of innovative technologies to increase access to care. By leveraging these technologies, we can have a greater focus on prevention, including comprehensive community-based services to address the social determinants contributing to young people’s wellbeing.
The development and wellbeing of young people occurs within dynamic concentric circles of influence exerted by different settings, namely: immediate family, supportive communities and the broader influences of the wider society. The influences of these spheres are interconnected and organised into seven domains, or social determinants of health: health, social support, education, employment, income and finance, housing and justice and safety.
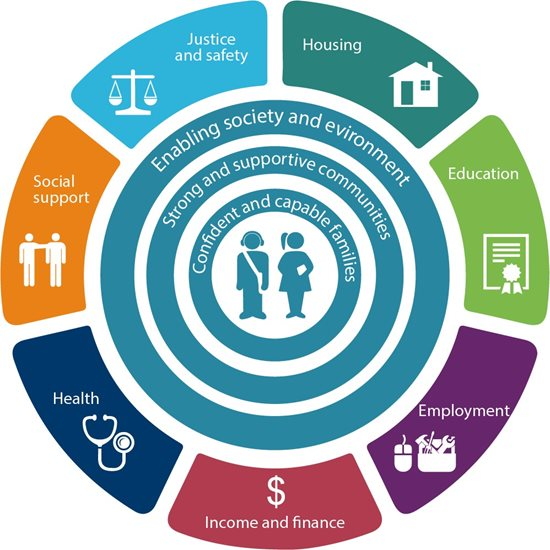
Figure 1: AIHW people-centred data model and an ecological approach to the wellbeing of young people (Source: Australia’s Youth, AIHW 2021)
In order for young people to thrive and flourish, they need to have all of these interconnected social determinants addressed appropriately and regularly. This goes beyond only seeing a medical professional – it means having a supportive network of friends, having hobbies and interests which nurture passions, working in a role or studying a discipline that sets one’s heart ablaze and finding a sense of belonging through community – either in-person or online.
… young people are concerned about their lack of voice in decision-making and in being negatively stereotyped.
Youth health advocates know this, but it is imperative for policy makers to consult with them so young people feature at the very core of proposed initiatives. This means collaborating and reflecting with children and young people so they are central to the design and delivery of services, strategies and approaches that affect them.
Unfortunately, recent data from UNICEF Australia has demonstrated that young people are concerned about their lack of voice in decision-making and in being negatively stereotyped. The proportion of young people aged 13-17 who think there is no clear way for children and young people to feed into the national discussion rose from 26% in April to 65% in July-August 2020.
Providing children and young people with a voice on their experiences has never been more important. These individuals need to be working hand-in-hand with policy makers to ensure services are personalised and interconnected across all of the seven domains. Young people have overwhelmingly suggested technology-based solutions to enhance convenience and offer an accessible stepping stone to connection with an ongoing face-to-face service. Social media could also be leveraged to promote awareness of service use and reduce the stigma associated with help-seeking.
When seeking support, young people still experience prejudice and discrimination, on account of cultural background, Aboriginality, sexuality, gender and age. Marginalisation makes access and navigation much more difficult due to the lack of relevant services, financial and practical support, and daily life challenges. Young people appreciate and need support to navigate systems through engagement with low-cost healthcare professionals, peers and community-based youth workers.
Professionals need to look beyond isolated encounters to consider the broader health and wellbeing needs of young people with significant advocacy roles. Youth-friendly service models underpinned by technology need to be integrated within the whole system navigation and then can be used to proactively support young people’s dynamic journeys throughout. Policy must acknowledge the voices of young people and provide training and support to professionals to optimise the untapped potential of technology. Our nation’s future depends on it.
About the author
 David Titeu is a youth health ambassador, member of the Youth Health Forum and CHF’s Mental Health Consumer Special Interest Group, where he takes part in consultations and helps push for better youth outcomes at a federal level. He is passionate about co-designed alternative models of care, peer support and social prescribing to address the social determinants of health. Having experienced mental health challenges as a consumer and young carer, David has been inspired to launch Linkmate, a social enterprise focused on proactive mental health support.
David Titeu is a youth health ambassador, member of the Youth Health Forum and CHF’s Mental Health Consumer Special Interest Group, where he takes part in consultations and helps push for better youth outcomes at a federal level. He is passionate about co-designed alternative models of care, peer support and social prescribing to address the social determinants of health. Having experienced mental health challenges as a consumer and young carer, David has been inspired to launch Linkmate, a social enterprise focused on proactive mental health support.
